Explainer: The Cuban Health Care System at Home and Abroad
Explainer: The Cuban Health Care System at Home and Abroad
The Cuban Revolution created a world-renowned health care model that’s free for Cubans—and incredibly profitable.
Cubans may lack basic goods, press freedoms, and smartphones, but they’ve got world-renowned health care. "We sincerely hope that all of the world's inhabitants will have access to quality medical services, as they do in Cuba,” said World Health Organization Director-General Margaret Chan in July 2014, adding that Cuba is “the only country that has a health care system closely linked to research and development.”
The Caribbean island’s preventive medicine model has afforded the country some of the best health statistics of the Western Hemisphere, including an infant mortality rate of 4.2 per thousand births—the lowest of all countries in the Americas—and a doctor-to-patient ratio of one physician per 150 Cubans (compared to one per 400 people in the United States). And even as the U.S. embargo prohibits Cuba from purchasing medical supplies or equipment that have at least 10 percent U.S. parts, the country has an internationally competitive biotech industry; it stands as Latin America’s largest pharmaceutical exporter and has developed one-of-a-kind vaccines.
The United States jumped on the island’s medical bandwagon in April, when New York Governor Andrew Cuomo’s trip to the island produced an agreement between the Roswell Park Cancer Institute of Buffalo and Cuba’s Center for Molecular Immunology. Now, the United States will conduct clinical trials of a Cuban lung cancer vaccine called CimaVax. In development since 1995, the drug has already been tested in 86 countries, including Australia, Peru, and the United Kingdom.
The State of Domestic Health
Cuba’s socialist medicine model has become the island’s most profitable sector through a cost-effective system at home and an international agenda for the poor.
Universal health care costs the government $300 per person every year, compared to the $7,000 spent on health care-related costs per person in the United States. This, however, comes at a cost to professionals’ salaries: doctors make $64 a month in the Caribbean country. In the meantime, the government makes over $8 billion a year from exporting health workers to natural disaster areas and poor communities around the world, such as the couple hundred doctors and nurses deployed to combat Ebola in West Africa last fall.
The framework for this internationalist approach dates back to the first years of the Cuban Revolution when 3,000 doctors—half of the island’s physicians—fled Cuba. The government responded by promoting medical careers at home, while also using new doctors to establish international relations and aid developing countries, performing millions of free operations and vaccinations. While these exports have fueled the Cuban economy more than any other industry, including tourism, it means 25,000 doctors are working abroad, bringing down the country’s celebrated doctor-to-patient ratio by a third.
Cuba is also home to the largest medical school in the world: Havana’s Latin American Medical School (ELAM), which former President Fidel Castro founded in 1998. United Nations Secretary-General Ban Ki-moon called it “the world's most advanced medical school.” So far, 23,000 students from more than 120 countries have graduated. ELAM graduates’ government-funded degrees stand in contrast to the mounting debt of U.S. medical students, averaging more than $176,000.
Major Programs Abroad: The Other Side of the Coin
The Ebola outbreak is only one recent case of Cuba’s experience handling crisis, the first dating back to Chile’s 1960 earthquake. Since then, 325,000 health workers have carried out missions in 158 countries—from Guatemala to Pakistan to Sri Lanka—according to Cuba’s Public Health Minister Dr. Roberto Morales Ojeda. In 2005, Castro even offered aid to the United States after Hurricane Katrina, though then-U.S. President George W. Bush refused.
But sending medical talent abroad also spells big bucks. Cuba’s export of medical talent in 2014 is expected to reel in $8.2 billion for the government. Yet, these professionals make only a fraction of that. As one Cuban ophthalmologist, Ileana González, told Al Jazeera, "Our salaries are very low. When you study medicine here it's for love, not money. You become a doctor because you want to help people—that's all."
For example, Brazil’s Mais Médicos (“More Doctors”) program brought in 4,500 Cuban doctors in 2014 with the goal of mitigating the South American country’s low physician-to-patient ratio, especially in rural areas. But the program has since become controversial given discrepancies of wages paid to these imported doctors. Brazil pays $4,200 for each of the health workers, of which the Cuban government keeps more than a third: Cubans are paid $400 a month, with another $600 deposited directly to bank accounts at home.
The system is Cuba’s carrot-and-stick method to keep doctors from defecting. For example, health workers in Venezuela also receive a minimal portion of the host country’s payments to the Cuban government; each earns $250 to $300 a month—a part of that frozen in an account on the island—out of Venezuela’s $10,000 a head contract, according to an article by Venezuelan journalist Alejandro Tarre in the Americas Quarterly Spring 2015 issue.
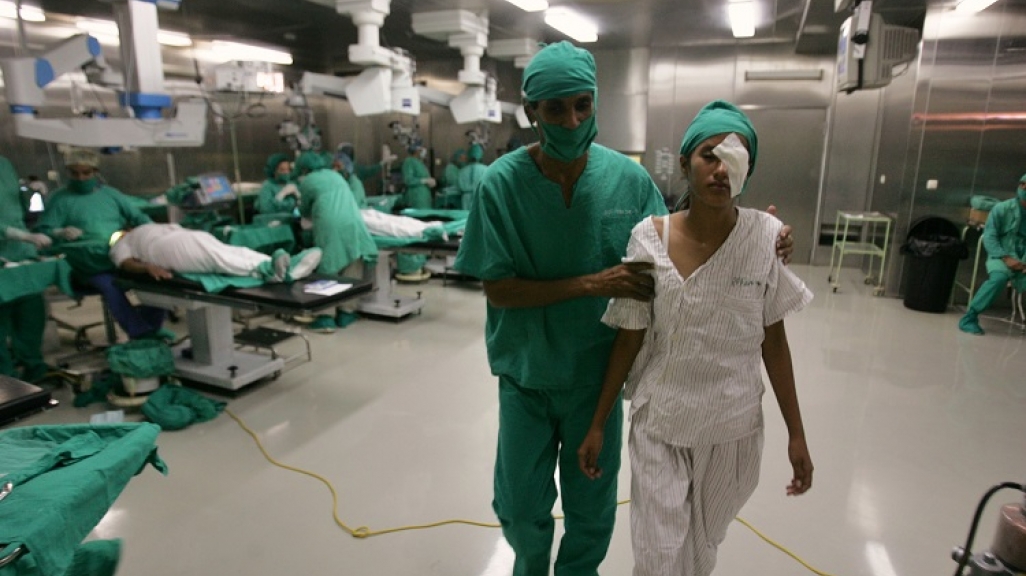
Doctors are central to the Cuba-Venezuela dynamic. Beginning in 2004, the two countries launched Operation Miracle, a humanitarian project to restore vision in especially impoverished communities by either providing people with eyeglasses and contact lenses or operations for free. In less than a decade, the program treated 1.5 million people, mostly from Latin America. Cuba receives approximately $3.5 billion in oil a year in exchange for the work of over 40,000 Cuban doctors in the Andean country—the largest portion of Cuban doctors working abroad. However, Venezuela’s deteriorating economy is one factor that is leading thousands to defect, usually to the United States. One report says only 22,000 Cuban physicians and nurses in Venezuela are left.
Cuba also has a track record of sending medical assistance to Africa, often coupled with military aid. A medical brigade to Algeria in 1963 marked the first of these cases, with 56 Cuban specialists sent to show “solidarity” with the newly independent African country. Ties remain strong with 900 medical technicians and doctors still there today. Plus, this week officials announced a new agreement to expand pharmaceutical trade between the two countries. The state pharmaceutical laboratory, Labiofam, is also responsible for vaccination campaigns across 15 West African countries. And by June 2015, the lab is set to finish constructing a facility in Tanzania that will help combat high rates of malaria there.
The remuneration of medical professionals in Africa has also been inconsistent. When the Ebola virus took hold of West Africa last year, Cuba sent 256 doctors and nurses—more health professionals than many developed countries. And while the international community praised the efforts of these health workers stationed across Sierra Leone, Liberia, and Guinea, the Cubans waited months before they received their first paychecks.